The Paper of the Month January
03 Jan 2022Can non-contrast computed tomography alone be used as an alternative to advanced imaging in selecting patients with late-presenting large-vessel occlusion for mechanical thrombectomy?
Title: Can non-contrast computed tomography alone be used as an alternative to advanced imaging in selecting patients with late-presenting large-vessel occlusion for mechanical thrombectomy?
Author: Prof. Anita Arsovska, Associate Commissioning Editor WSA
This article is a commentary on the following
Summary:
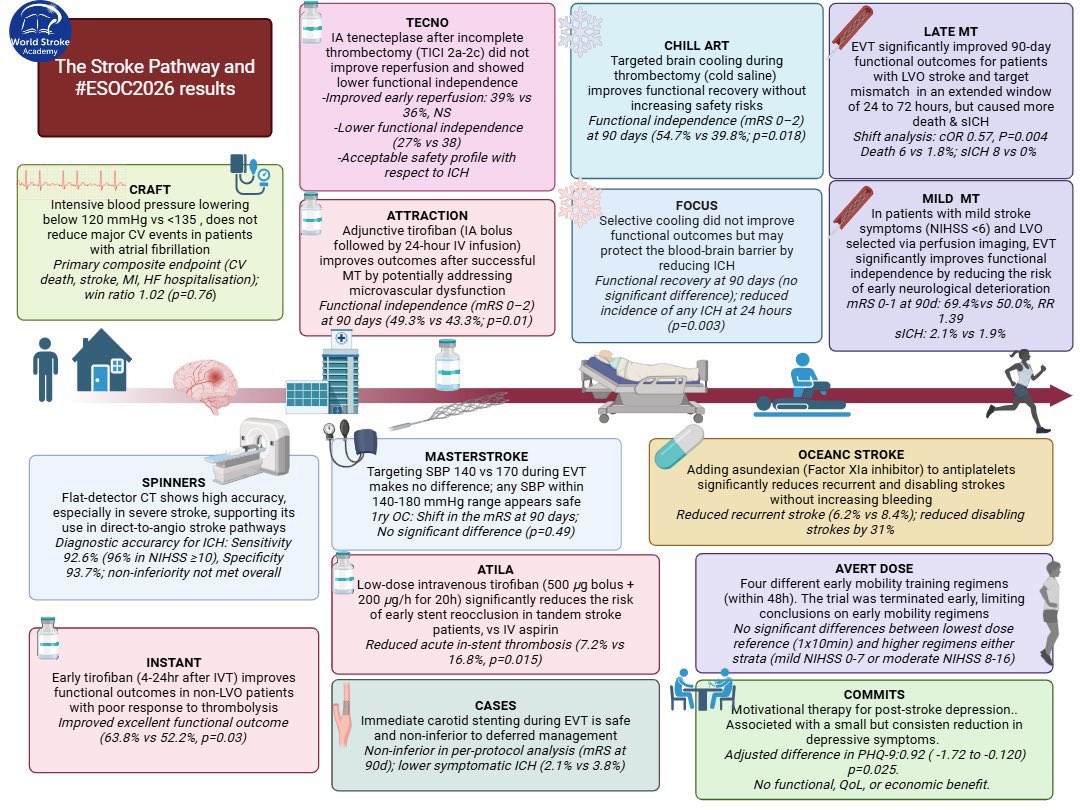
The CT for Late Endovascular Reperfusion (CLEAR) study was a multicenter cohort study of consecutive patients with proximal anterior circulation stroke undergoing mechanical thrombectomy (MT) in the extended time window, defined as a period from TLSW to arterial puncture between 6 to 24 hours¹. This study was conducted at 15 sites across 5 countries in Europe and North America. The duration of follow-up was 90 days from stroke onset. Clinical outcomes of patients selected for mechanical thrombectomy by non-contrast computed tomography (CT) vs those selected by computed tomography perfusion (CTP) or magnetic resonance imaging (MRI) in the extended time window were compared.There was no difference in 90-day ordinal mRS shift between patients selected by CT vs CTP (adjusted odds ratio [aOR], 0.95 [95% CI, 0.77-1.17]; P = .64) or CT vs MRI (aOR, 0.95 [95% CI, 0.8-1.13]; P = .55). The rates of 90-day functional independence (mRS scores 0-2 vs 3-6) were similar between patients selected by CT vs CTP (aOR, 0.90 [95% CI, 0.7-1.16]; P = .42) but lower in patients selected by MRI than CT (aOR, 0.79 [95% CI, 0.64-0.98]; P = .03). Successful reperfusion was more common in the CT and CTP groups compared with the MRI group (474 [88.9%] and 670 [89.5%] vs 250 [78.9%]; P < .001). No significant differences in symptomatic intracranial hemorrhage (CT, 42 [8.1%]; CTP, 43 [5.8%]; MRI, 15 [4.7%]; P = .11) or 90-day mortality (CT, 125 [23.4%]; CTP, 159 [21.1%]; MRI, 62 [19.5%]; P = .38) were observed. The authors conclude that there were no significant differences in the clinical outcomes of patients selected with non-contrast CT compared with those selected with CTP or MRI. This could potentially widen the indication for treating patients in the extended window using a simpler and more widespread non-contrast CT.
Commentary:
Current guidelines still recommend use of advanced imaging in stroke patients with anterior LVO presenting beyond 6 hours who are candidates for mechanical thrombectomy (refs).The 2018 AHA/ASA Guidelines suggestthat in selected patients with a large vessel occlusion within 6-24 hours from last known normal who would also have been eligible for DAWN or DEFUSE 3, obtaining perfusion imaging (CT-P or MR-P) or an MRI with diffusion-weighted imaging (DWI) sequence is recommended to help determine whether the patient is a candidate for mechanical thrombectomy². Similarly, the 2019 ESO/ESMINT Guidelines advise that in adult patients with anterior circulation LVO-related acute ischaemic stroke presenting beyond 6 hours from time last known well, advanced imaging selection is necessary (with moderate quality of evidence and strong strength of recommendation³).
Kim et al. (2019) aimed to elucidate whether MRI-based selection for EVT is safe and effective within and after a 6-hour time window compared with conventional CTA-based selection⁴.Their study found that MRI-based selection for EVT was not associated with improving functional outcome compared with CT-based selection, but might be better at reducing the risk of SICH, despite the delays in all workflow time metrics.
Bouslama et al. (2021) compared the prediction of post-reperfusion infarct volumes and the clinical outcomes across NCCT e-Stroke software versus RAPID (IschemaView, Menlo Park, CA) computed tomography perfusion measurements⁵.Baseline ischemic core volumes measured by e-Stroke Suite software on NCCT performed similarly to RAPID CTP in estimating post-full reperfusion infarct volumes and functional outcomes for both early- and late-presenting patients. It was concluded that NCCT e-ASPECTS software volumes could be used along CTP to further refine selection for thrombectomy and could also represent a viable alternative in centers where access to advanced imaging is limited.
Jadhav et al. (2021) aimed to compare post-EVT outcomes between patients who underwent pre-randomization basic (non-contrast computed tomography [CT], CT angiography only) versus additional advanced imaging (computed tomography perfusion [CTP] imaging) and to determine the association of performance of pre-randomization CTP imaging with clinical outcomes⁶. They analyzed 1348 patients, 610 (45.3%) of whom underwent CTP pre-randomization. The benefit of EVT compared with best medical management was maintained irrespective of the baseline imaging paradigm. There was no difference between the CTP and non-CTP group (17.1% vs 16.1%) (p=0.57). The 90-day modified Rankin Scale score 0–2 in EVT versus control patients was 46.0% (137/298) in the CTP group versus 28.9% (88/305), whereas 44.1% (162/367) in the without CTP group versus 27.3% (100/366) in the control group. Performance of CTP baseline imaging compared with baseline non-contrast CT and CT angiography only yielded similar rates of good outcome (odds ratio, 1.05 [95% CI, 0.82–1.33], adjusted odds ratio, 1.04, [95% CI, 0.80–1.35]).The authors conclude that rates of good functional outcome were similar among patients in whom CTP was or was not performed, and EVT treatment effect in the 0- to 6-hour time window was similar in patients with and without baseline CTP imaging.
Conclusion:
Based on the latest clinical trials, non-contrast computed tomography alone maybe used as an alternative to advanced imaging in selecting patients with late-presenting large-vessel occlusion for mechanical thrombectomy. More data are needed on specific inclusion and exclusion criteria of potential patients.
References:
- Nguyen TN, Abdalkader M, Nagel S, et al. Noncontrast Computed Tomography vs Computed Tomography Perfusion or Magnetic Resonance Imaging Selection in Late Presentation of Stroke With Large-Vessel Occlusion. JAMA Neurol.Published online November 08, 2021. doi:10.1001/jamaneurol.2021.4082
- Powers WJ, Rabinstein AA, Ackerson T, et al., on behalf of the American Heart Association Stroke Council. 2018 Guidelines for the Early Management of Patients With Acute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke2018;49:e46-e110.
- Turc G, Bhogal P, Fischer U, et al. European Stroke Organisation (ESO)—European Society for Minimally Invasive Neurological Therapy (ESMINT) guidelines on mechanical thrombectomy in acute ischaemic stroke endorsed by Stroke Alliance for Europe (SAFE). Eur Stroke J. 2019;4(1):6-12. doi:1177/2396987319832140.
- Kim JT, Cho BH, Choi KH et al. Magnetic Resonance Imaging Versus Computed Tomography Angiography Based Selection for Endovascular Therapy in Patients With Acute Ischemic Stroke. Stroke 2019; 50:365-372. https://doi.org/10.1161/STROKEAHA.118.023173
- Bouslama M, Haussen DC, Rodrigues G, Barreira C, Frankel M, Nogueira RG. Novel selection paradigms for endovascular stroke treatment in the extended time window. J Neurol Neurosurg Psychiatry. 2021;jnnp-2020-325284. doi:1136/jnnp-2020-325284
- Jadhav PA, Goyal M, Ospel J et al. Thrombectomy With and Without Computed Tomography Perfusion Imaging in the Early Time Window: A Pooled Analysis of Patient-Level Data. https://doi.org/10.1161/STROKEAHA.121.034331 2021;0:STROKEAHA.121.034331
Author Interview
Thanh Nguyen, MD, FRCP, FSVIN, FAHA
1. WHAT DID YOU SET OUT TO STUDY?
Our research question was as follows:
In patients with a large vessel occlusion stroke presenting in the late 6-24 hour time window, do patients selected for mechanical thrombectomy with non-contrast head CT have 3-month outcomes comparable to patients who are selected by advanced imaging with CTP or MRI?
2. WHY THIS TOPIC?
In 2017-2018, the DAWN and DEFUSE3 trials demonstrated significantly improved outcomes for patients treated with clot retrieval presenting in the late 6-to-24-hour time window from symptom onset, compared to best medical management. In both studies, advanced imaging with CT perfusion or MRI were utilized to select patients into these trials.
Subsequent to the publication of these two landmark trials, the American Heart/ Stroke Association, the European Stroke Organization guidelines recommended that patients with large vessel occlusion presenting in the late window should be selected for thrombectomy treatment based on the advanced imaging triage paradigms that were utilized in the DAWN and DEFUSE3 studies.
However, advanced imaging with CT perfusion or MRI is not widely available in many centers across the world, and as such, many patients are not being treated for lack of this technology. We have confirmed this being true in centers in Central America, South America, the United Kingdom, Asia (China), and Africa. Of note, these advanced imaging studies can be resource intensive for a center and costly.
If we could show that a more widely available imaging study, i.e. non-contrast head CT, would demonstrate similar outcomes as compared with advanced imaging, then our hope was to open the treatment paradigm to late window patients who present at centers without available advanced imaging.
3. WHAT WERE THE KEY FINDINGS?
The key findings were that in patients with large vessel occlusion of the carotid terminus or proximal middle cerebral artery (M1/M2 segments), presenting in the late (6 to 24 hour) time window from symptom onset, patients who are selected for treatment using non-contrast head CT have similar outcomes compared to patients who are selected with advanced imaging.
It is important to note that in patients who were selected using non-contrast head CT for intervention, they had very little evidence of brain infarction on their CT scan, as measured by the ASPECTS score. The same is true for patients who were selected by advanced imaging, they also had very little evidence of brain infarction. The median ASPECTS of patients in this study was 8, with IQR lower border to 7.
Furthermore, in an analysis of patients who presented directly to an endovascular-capable center, (i.e. mothership patients), patients who were selected with non-contrast head CT had faster times to treatment compared to patients selected with advanced imaging with CTP or MRI.
4. HOW MIGHT THESE RESULTS IMPACT CLINICAL PRACTICE?
This is important because the paradigm or workflow selection of patients presenting with large vessel occlusion in the late window could be simplified by triage with a non-contrast head CT as an alternative to advanced imaging studies.
This alternative may broaden the indication for treating patients in centers where no advanced imaging is available. It will also decrease significantly the cost and time for patients undergoing endovascular treatment.
5. WHAT SURPRISED YOU MOST?
I was intrigued that patients who had more distal occlusion (i.e., M2 occlusion) had more utilization of CT perfusion compared to patients with more proximal occlusion (i.e. M1 or carotid terminus), who were commonly selected with non-contrast head CT.
This suggests that in patients presenting with a higher severity of illness with more proximal occlusions, physicians may have a lower threshold to accept triage of these patients to intervention with non-contrast head CT only.
6. WHAT’S NEXT FOR THIS RESEARCH?
We await the result of two other randomized trials which ask whether selection of patients with large vessel occlusion presenting in the late window, with head CT imaging (with CTA collateral assessment) demonstrates benefit compared to medical management of these patients.
We also await the results of several ongoing large infarct core trials examining whether thrombectomy is of benefit to patients compared to medical management. A non-contrast head CT is being used in the paradigm of selection for a subset of these studies.
7. IS THERE ANYTHING YOU’D LIKE TO ADD?
I’d like to thank our many colleagues, co-authors for contributing to this study, and to Oscar Bolanos for funding support from Medtronic. I’d like to thank the Society of Vascular and Interventional Neurology for pilot grant funding.
VIDEO INTERVIEW: